



Emily Jerry - 2 yo Girl

Emily - 24 months old girl. Diagnosed with yolk sac tumor in abdomen at 18 months. Treated with chemotherapy, latest MRI shows Emily clear of cancer. In hospital to receive final round of chemotherapy.

Initial Assessment
What do you think is going on with this patient?
(everyone to answer)
Initial Assessment ( ~3 min)
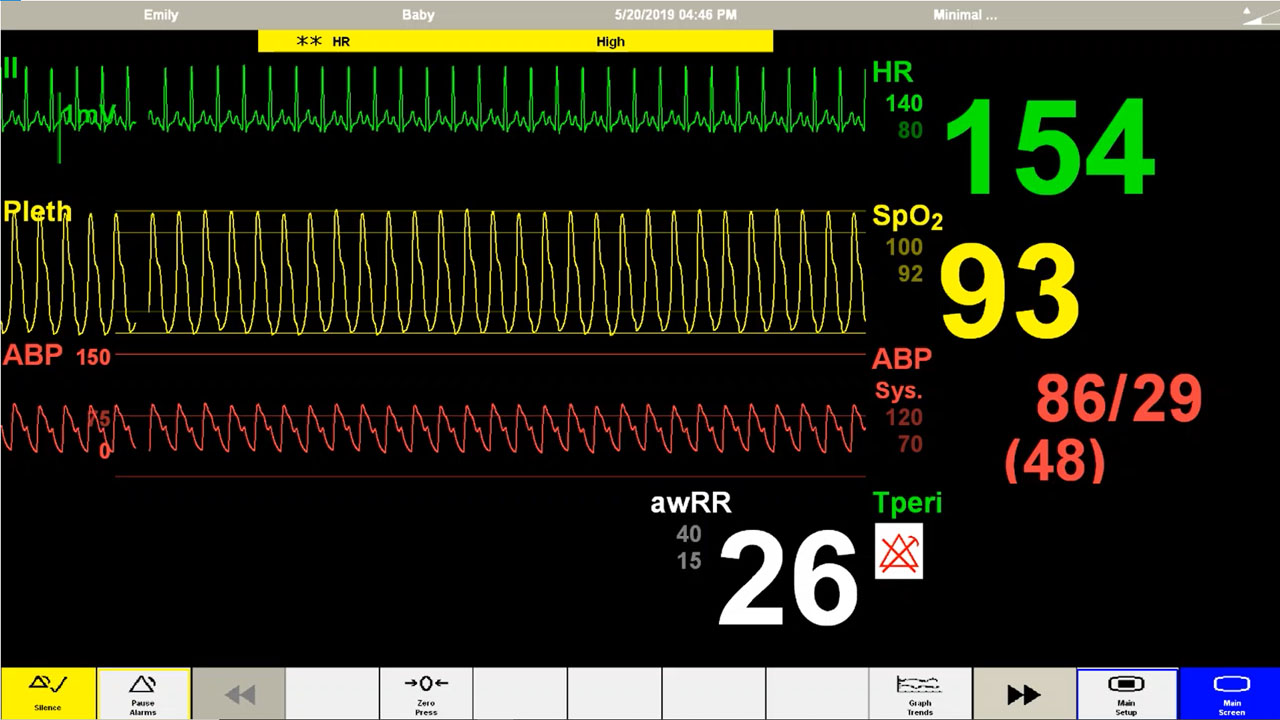
Final round of chemotherapy treatment beginning to be administered via IV.
Emily starts screaming in pain that her head hurts, vomiting. Urgent call for help by mother.
Emily starts screaming in pain that her head hurts, vomiting. Urgent call for help by mother.


Assessment Review
Share what you are most concerned about.
(everyone to answer)
Review Assessment ( ~3 min)
5 minutes later ...
Patient unconscious and in cardiac arrest
Patient unconscious and in cardiac arrest

Emily's Story

Summary:
Emily had no brain activity shorty after Feb 26, 2006 (3rd day of her chemotherapy treatment).
Emily's chemotherapy treatment was compounded using concentrated sodium chloride solution instead of a standard bag of sodium chloride solution (23.4% vs less than 1% sodium chloride).
Pharmacy technician, unable to find a standard prepared bag and unaware of the impact, compounded using the concentrated sodium chloride solution.
Emily had no brain activity shorty after Feb 26, 2006 (3rd day of her chemotherapy treatment).
Emily's chemotherapy treatment was compounded using concentrated sodium chloride solution instead of a standard bag of sodium chloride solution (23.4% vs less than 1% sodium chloride).
Pharmacy technician, unable to find a standard prepared bag and unaware of the impact, compounded using the concentrated sodium chloride solution.

Systems Discussion
What systems do we have in place to prevent this?
(every team member to answer)
(every team member to answer)
What system issues might have contributed to this outcome?
(every team member to answer)
(every team member to answer)
Systems Discussion (~5 min)
Issues:
- incorrect medication dosage
- manual compounding of medication
- medication shortage (run out of standard bag)
- pharmacy technician lacking clinical knowledge
- incorrect medication dosage
- manual compounding of medication
- medication shortage (run out of standard bag)
- pharmacy technician lacking clinical knowledge

