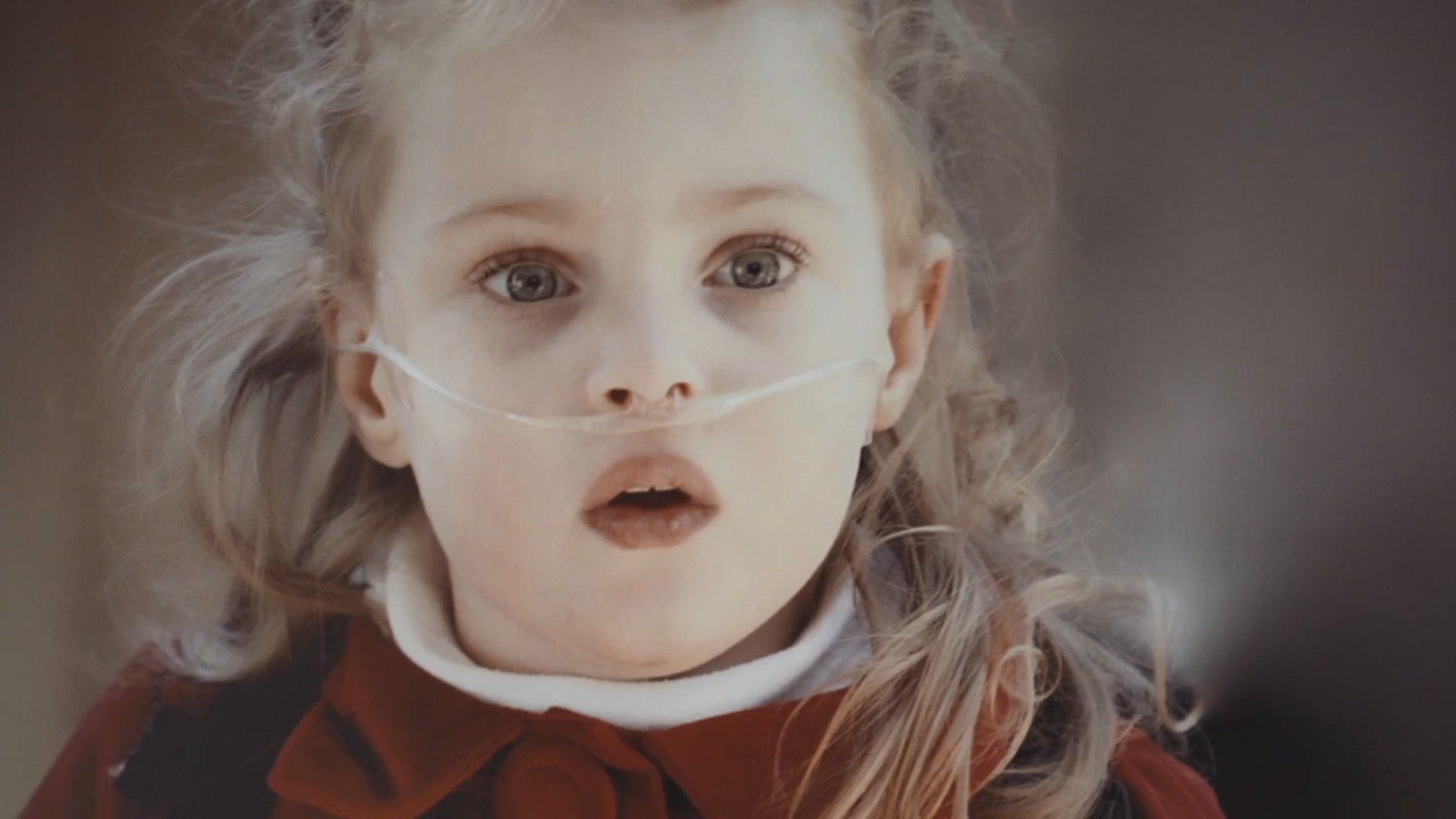






Nora - 3 yr old girl
Nora - 3 year old girl diagnosed with pulmonary hypertension ("PH"). Nora needed to be on oxygen 24/7 and take oral vasodilators to help reduce pressure in her lungs.

Initial Assessment
What do you think is going on with this patient?
(everyone to answer)
Initial Assessment ( ~3 min)
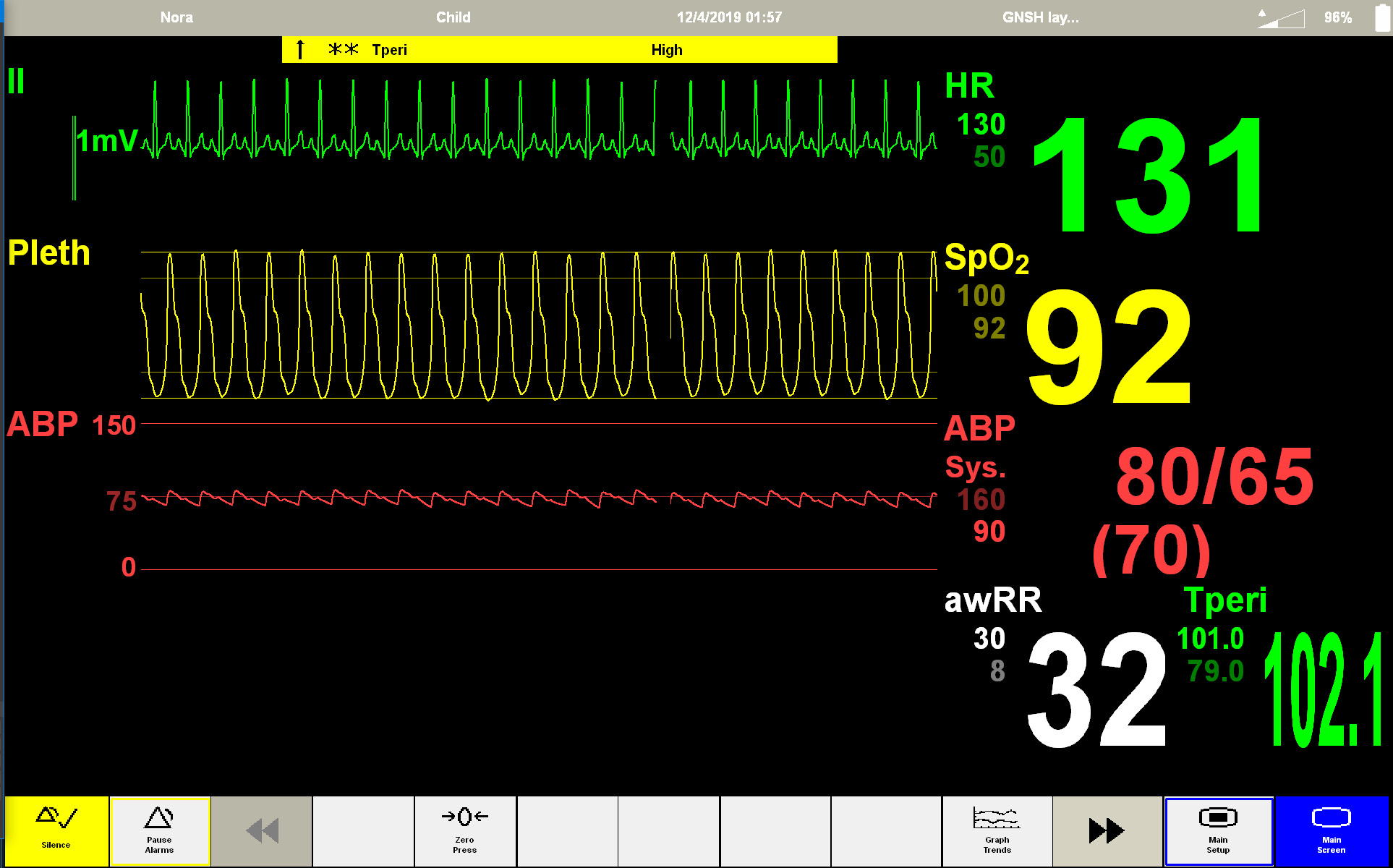
As her PH worsened, she needed IV vasodilators. Shortly after getting the central line for her IV vasodilators, Nora developed an allergy to something in the dressing change kit. Dressing change protocol changed. Within 2 months Nora developed a central line infection. Central line removed; temporary central line placed in her arm. Day after sent home, that line had signs of infection. When the second line pulled lots of pus evident.

Review Assessment
Share what you are most concerned about.
(everyone to answer)
Review Assessment ( ~3 min)
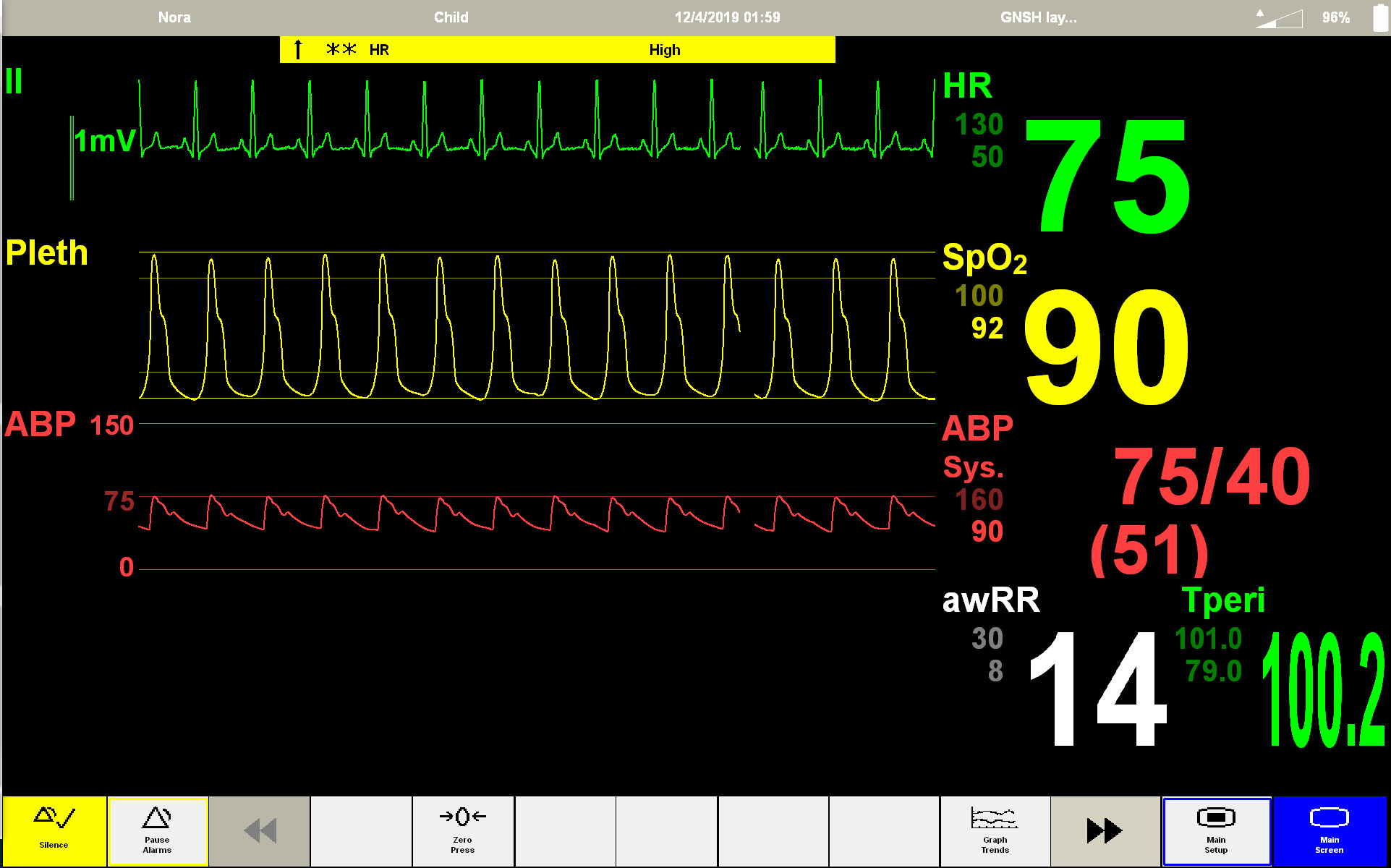
Placed on subcutaneous Remodulin but she did not do as well. Fainted, went to ER, dehydration, acute heart failure. Survived but spent 70 days in ICU.
Received another central line. Family noticed nursing staff not following central line protocol for dressing change. 6 weeks later developed another central line infection. Line replaced with a tunneled line in chest. Within 32 hours, that site infected – IV antibiotics.
Two months later, fainted, taken to hospital. Nora had a fever within 48 hours in hospital – she had contracted croup. By that night in septic shock. Across next two weeks, other preventable harm events occurred: received double dose of diuretic which sent her into acute dehydration and heart failure; parental nutrition inadvertently stopped for 3 days.
Received another central line. Family noticed nursing staff not following central line protocol for dressing change. 6 weeks later developed another central line infection. Line replaced with a tunneled line in chest. Within 32 hours, that site infected – IV antibiotics.
Two months later, fainted, taken to hospital. Nora had a fever within 48 hours in hospital – she had contracted croup. By that night in septic shock. Across next two weeks, other preventable harm events occurred: received double dose of diuretic which sent her into acute dehydration and heart failure; parental nutrition inadvertently stopped for 3 days.

Patient Declining
Infection
Share what you are most concerned about.
(everyone to answer)
Review Assessment ( ~3 min)
2 weeks later ...
Skin white with bluish discoloration around mouth, central cyanosis
- O2 via non-rebreather mask
- HR: undetectable; agonal heart rythm
- BP: undetectable
- SPO2: undetectable
- Respirations: agonal breathing
- Code Blue Called ...
Skin white with bluish discoloration around mouth, central cyanosis
- O2 via non-rebreather mask
- HR: undetectable; agonal heart rythm
- BP: undetectable
- SPO2: undetectable
- Respirations: agonal breathing
- Code Blue Called ...
Nora's Story

Summary:
Nora died on November 22, 2013
Nora died from preventable healthcare errors.
Nora died on November 22, 2013
Nora died from preventable healthcare errors.
Team Discussion
What can our team learn from this case to improve the care in a similar situation?
Team Discussion (~5 min)
Systems Discussion
What systems do we have in place to prevent this?
(every team member to answer)
(every team member to answer)
What system issues might have contributed to this outcome?
(every team member to answer)
(every team member to answer)
Systems Discussion (~5 min)
Issues:
- infection control
- adherence to central line insertion and care protocols
- infection control
- adherence to central line insertion and care protocols
